 As soon as your pregnancy is confirmed it is recommended that you find and register with a lead maternity carer (LMC), by nine weeks gestation, if possible.
As soon as your pregnancy is confirmed it is recommended that you find and register with a lead maternity carer (LMC), by nine weeks gestation, if possible.
Your LMC will organise your first booking visit (before 12 weeks gestation) to review your general wellbeing, provide dietary advice, explain options for antenatal screening, arrange appropriate tests and discuss support services.
West Coast based midwives providing primary care
Self-employed LMC midwives provide both hospital and home births. If you are thinking of having a homebirth or would like more information on home birth, view our Home Birth Association information, and visit the findyourmidwife site for LMC midwives who facilitate home births.
Find Your Midwife
Antenatal Tests and Screening
What is a first trimester screening test?
Maternity care providers will often suggest a pregnant mother has a blood test taken when she is 10 weeks pregnant. This is specifically to conduct a measurement of pregnancy hormones. If chromosomal abnormalities are present, these results can be out of the normal range.
These blood tests, in combination with the 12 week ultrasound, provide what is known as “A First Trimester Screening Test”. A mother’s age, including the results from the blood test, and the findings of the ultrasound all provide an individualised picture of her risk of having a baby with Down Syndrome. This screening test is not a definite diagnosis of chromosomal problems, but rather provides a risk assessment. If there are concerns, then further testing can be done.
Please register with your LMC within at least the first 10 weeks to ensure your antenatal scans can be booked at Te Nīkau, Grey Hospital & Health Centre.
Late booking of antenatal scans may require travel to Christchurch at your own cost.
Click here to access West Coast based LMCS
12 Week Ultrasound Scan
If you have not yet had any type of pregnancy ultrasound and you are around 12 weeks pregnant, your maternity care provider may suggest you have one. There are many reasons for having an ultrasound at this stage, but one of the most common is to screen for one of the congenital chromosomal abnormalities – Trisomy 21, otherwise known as Down Syndrome. This means that there is an extra chromosome – 21 contained in every cell of the body.
People with Down Syndrome have physical and intellectual disabilities. Older women are more at risk of having a baby with Down Syndrome.
When a woman is 12 weeks pregnant her risk of having a baby with Down Syndrome can be fairly accurately assessed. When a foetus has Down syndrome they tend to have more fluid at the base of their neck, in the region known as the nuchal fold area. This fluid can be measured in a test called nuchal translucency. A foetus with Down Syndrome has a measurement which is thicker than in those who do not.
It is worth remembering though, that a larger than average nuchal fold measurement is not a guarantee that the baby will have chromosomal problems. Other tests for Down Syndrome need to be done if in doubt. In addition, blood tests such as a Chorion Villus Sampling test or an amniocentesis help to clarify any suspicions.
I can see my baby! – but…
The 12 week ultrasound may be the first time parents have seen their little baby. So this is an exciting, if a little nerve-wracking time. It’s completely normal for parents to consider the possibility that their baby may not be developing as it needs to and perhaps build apprehension before the procedure. After all, this is one of the reasons why a 12 week ultrasound is recommended.
One of the benefits of having an ultrasound so early in pregnancy is that if complications are found, then parents may be given a choice of continuing with the pregnancy or not. Medical recommendations around this issue are very important. Ethical, religious and personal belief systems also need to be carefully balanced and weighed up.
Parents need to feel as if they are fully informed and comfortable with the explanations provided by the sonographer doing the 12 week ultrasound. Follow up care by the healthcare team are equally as important.
How will they do the 12 week ultrasound?
The 12 week ultrasound is generally done via the mother’s abdomen. It’s not always necessary to have a full bladder, however the individual sonographer may recommend that you have a partially full bladder. This will help to lift your uterus up out of your pelvis so it is easier to see the foetus. Sometimes it is necessary to do a vaginal ultrasound. This will lead to even clearer images.
Reasons to have a 12 week ultrasound
- To check that the foetus is developing as it should be. The measurements of the foetus’s skull – the Biparietal distance is calculated and compared against standard lengths for foetuses at similar gestational ages.
- To see if the foetus has a heartbeat. This should be clearly detectable at the 12 week ultrasound.
- To confirm pregnancy dates and estimate the date of delivery.
- To check for multiple foetuses and confirm if one or more is present.
- To check the size of the foetus and developing placenta.
- To measure the amount of fluid at the base of the foetus’s neck and make an individualised risk assessment of them having Down Syndrome. The sound waves from the ultrasound return echo free measurements. This is because of the space which is translucent due to its fluid content.
- To check for other physical abnormalities in the foetus.
- To check the uterus, fallopian tubes and pelvic region for other complications.
What else is measured during a 12 week ultrasound?
- The foetus’s length, specifically from its head to its bottom. This is known as a Crown Rump length.
- A general check of the mother and foetus’s internal organs and structures.
Many parents are amazed by the amount of detail they can see at the 12 week ultrasound. They are also surprised by their foetus’s movements and agility. Of course, at 12 weeks gestation it is too early for a pregnant mother to be aware of her baby moving. And it can be a strange sensation when looking at the monitor and seeing movement but not being able to physically detect it.
Many parents feel an instant emotional connection with their baby when they see it for the first time. It’s not uncommon for fathers to say that until they 12 week ultrasound, the whole pregnancy idea was a little foreign and somehow not real. But being able to see their baby rather than talking about it and having to use their imagination, makes all the difference.
When will I know if everything’s alright with my 12 week ultrasound?
You should be told straightaway if everything is going well. If you have had your biochemistry blood tests taken before the ultrasound and these results are back, then you should be able to have these results as well straight after your ultrasound is finished or at your next appointment with your maternity carer. Many maternity healthcare providers recommend mothers have the blood test at 10 weeks gestation.
The sonographer will be able talk their way through the procedure and turn the screen so that you can see what they are looking at during the ultrasound. There may also be a separate monitor for you and your partner to look at. If you want explanation, then just ask the sonographer to tell you what they are checking.
If they are unsure or want clarification they will often request a colleague come into the room and have a look at the ultrasound. Obviously, this can be a pretty unnerving process especially if you’ve not had any reason to believe that there are any complications.
How accurate is the first trimester screening test?
At the current time, the combined First Trimester Screening is thought to be the most accurate test for Down Syndrome. For those women whose results return a high risk of carrying an embryo with Down Syndrome the next stage is generally Chorionic Villus Sampling or an Amniocentesis.
Having a low risk result for the First Trimester Screening Test does not give a 100% guarantee that there will not be a chromosomal abnormality. What it does is categorise a pregnancy into an increased or decreased risk.
How long will my 12 week ultrasound take?
Generally, bookings of 30 minutes are made. This allows the sonographer enough time to do a thorough and comprehensive check and assessment. Try not to squeeze your appointment time between a lot of other tasks you need to achieve in the same day.
Put aside some time before and after your ultrasound so you can make it to the appointment in plenty of time, and have the chance to reflect on it afterwards. Ask your partner to be with you on the day, and aim to enjoy this as an event you can both share.
Some couples choose to bring family members along as well, and view this as an opportunity to meet their new family member for the first time. How you manage this is your choice, just be mindful that ultrasound rooms can be quite small, so accommodating more than a couple of people can present a practical challenge.
Are 12 week ultrasounds part of my routine pregnancy care?
Ultrasounds during pregnancy are routinely offered because they provide such an excellent means of diagnosing problems if they are present. They are also low risk, non –invasive and relatively low cost considering the amount of information they give. But you are entirely free to make your own choices regarding whether you want to have pregnancy ultrasounds or not.
Some parents feel very strongly that having an ultrasound is not right for them. Part of their reasoning is that if abnormalities are found, then they may be put into a position of having to make decisions based around these findings and for this reason a consent form is completed before this scan is undertaken to ensure this is a scan you actually want to have done.
Some parents choose to wait until the screening ultrasound at 18-20 weeks and feel that at 12 weeks it is still too early to be able to see much of their baby’s development. If you are in any doubt, then speak with your maternity care provider about your own individual needs.
For more information on antenatal tests and screening, refer to HealthInfo
Postnatal Visits
The LMC who looked after you during your pregnancy will provide postnatal visits after the birth. The LMC provides care for the first six weeks of the post natal period, then will refer you and baby to the GP and Well Child Provider you have chosen. If you live in a rural area where there is no Well Child provider the Rural Nurse Specialist will provide ongoing care and support.

 As soon as your pregnancy is confirmed it is recommended that you find and register with a lead maternity carer (LMC), by nine weeks gestation, if possible.
As soon as your pregnancy is confirmed it is recommended that you find and register with a lead maternity carer (LMC), by nine weeks gestation, if possible.



 The West Coast Nutrition service is staffed by NZ registered dietitians and is available for women using Maternity Services on the West Coast. Working Monday to Friday staff see women as outpatients and inpatients for individualised nutrition assessment and advice.
The West Coast Nutrition service is staffed by NZ registered dietitians and is available for women using Maternity Services on the West Coast. Working Monday to Friday staff see women as outpatients and inpatients for individualised nutrition assessment and advice.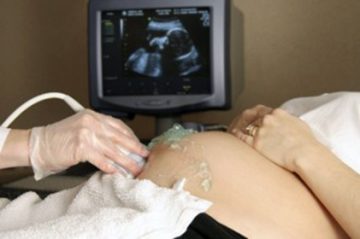 The Te Nīkau, Grey Hospital & Health Centre Radiology Department provides ultrasound scanning for pregnant women. Your LMC midwife or doctor will refer you to this service. To ensure timeliness of appropriate ultrasound screening it is important that your referral is made to the Radiology Department before 11 weeks of pregnancy.
The Te Nīkau, Grey Hospital & Health Centre Radiology Department provides ultrasound scanning for pregnant women. Your LMC midwife or doctor will refer you to this service. To ensure timeliness of appropriate ultrasound screening it is important that your referral is made to the Radiology Department before 11 weeks of pregnancy. Professional cultural services – visits from local Kaumātua can be initiated on your behalf for such things as karakia, tikanga support, cultural guidance, guidance on issues of tapu and tangihanga support.
Professional cultural services – visits from local Kaumātua can be initiated on your behalf for such things as karakia, tikanga support, cultural guidance, guidance on issues of tapu and tangihanga support. The West Coast Breastfeeding Handbook (as pictured on the right) was developed with help of many West Coast mums and launched in August 2012 and last updated in March 2019.
The West Coast Breastfeeding Handbook (as pictured on the right) was developed with help of many West Coast mums and launched in August 2012 and last updated in March 2019.
 This screening programme is designed for early detection of babies with moderate to severe hearing loss. The West Coast DHB has two fully trained and certified newborn hearing screeners – Barbara Roberts and Mary Sullivan, both based at Te Nīkau, Grey Hospital & Health Centre.
This screening programme is designed for early detection of babies with moderate to severe hearing loss. The West Coast DHB has two fully trained and certified newborn hearing screeners – Barbara Roberts and Mary Sullivan, both based at Te Nīkau, Grey Hospital & Health Centre.